The Bottom Line: Your Home Floors Are Not Your Friends
If you have plantar fasciitis, going barefoot on hard floors can keep your heel irritated all day.
Supportive slippers (or house shoes) help by giving you arch support, heel stability, and cushioning every time you take a step — which adds up fast at home.
Disclosure: This post may contain affiliate links. If you buy through them, we may earn a small commission at no extra cost to you.
Home isn’t just where the heart is…
Home is supposed to be your safe zone.
And then plantar fasciitis shows up and says, “Nice hardwood floor you’ve got there… would be a shame if someone made it feel like cactus.”
If you’re limping around the kitchen, dodging chores, or doing the “toe-walk of denial” to avoid heel pain, this post is for you.
Because the fix is often hilariously simple: stop raw-dogging your floors.
Want the big picture? Start here: Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
1) Why Going Barefoot at Home Can Make Plantar Fasciitis Worse
Plantar fasciitis is commonly aggravated by repeated strain and impact, especially on hard surfaces.
That’s why conservative treatment guidance often includes supportive footwear and, for many people, inserts/orthotics.
At home, the problem is simple: you take a lot of “little steps” — and they add up.
References:
Mayo Clinic: Plantar Fasciitis (Diagnosis & Treatment) | Cleveland Clinic: Plantar Fasciitis
Lisa’s tale: “My third bout of PF literally started because I insisted on going barefoot indoors. Big mistake.”
Action Box: The 10-Second Home Test
- [ ] Do I feel worse after walking barefoot on tile/hardwood?
- [ ] Is my first step in the morning brutal?
- [ ] Do I stand a lot in the kitchen (hard floor = heel impact city)?
- [ ] Do my feet feel “tired” fast indoors?
If you checked any of those: supportive slippers are not a luxury. They’re a daily-defense tool.
2) What to Look For in Supportive Slippers (The PF Checklist)
- Real arch support: contoured footbed (not just “soft foam”).
- Heel cup or heel cradle: keeps your heel stable and reduces sloppy motion.
- Secure fit: straps/upper that holds your foot — no floppy “shuffle slippers.”
- Cushioning that doesn’t collapse: especially under the heel.
- Indoor/outdoor sole (optional): helpful if you step outside (mailbox missions, dog duty).
Bob’s tip: “I used to shuffle in backless slippers like a zombie. Now I pick ones with a slight heel cup so I’m not waddling.”
3) Slippers vs House Shoes (Yes, There’s a Difference)
- Slippers: usually softer, more “lounge.” Some are backless (mules), which can be less stable.
- House shoes: more structured, often with a firmer sole and better heel containment — closer to a lightweight indoor sneaker.
Translation: slippers are for Netflix marathons. House shoes are for kitchen marathons.
Both can work — as long as they’re supportive.
4) Supportive Slippers & House Shoes
These are the kinds of supportive indoor options people often look at first when heel pain is getting aggravated at home.
- Orthotic-friendly, supportive: OrthoFeet slippers / house shoes
- Deep heel cup + support slide: Spenco supportive slides
- Cozy moc with a sturdier sole: Acorn moc slippers
Lisa’s note: “OrthoFeet’s plush lining is basically a foot hug — and the support keeps my heel from getting cranky by noon.”
5) Make Your Slippers Work Harder (Fit + Habits)
- Replace flattened footbeds: when support collapses, pain often returns.
- Rotate pairs: if you’re in slippers all day, alternating reduces wear and helps cushioning rebound.
- Add inserts if removable: some house shoes accept OTC or custom orthotics nicely.
- Don’t shuffle: if your slipper forces you into a “toe-grip shuffle,” switch styles.
If you want to go deeper on inserts, see our Why Insoles Matter for Plantar Fasciitis in 2026 guide.
Small home habit that helps: a quick calf stretch (morning and evening) can reduce the pull on the plantar fascia.
Harvard Health commonly notes stretching as part of conservative approaches.
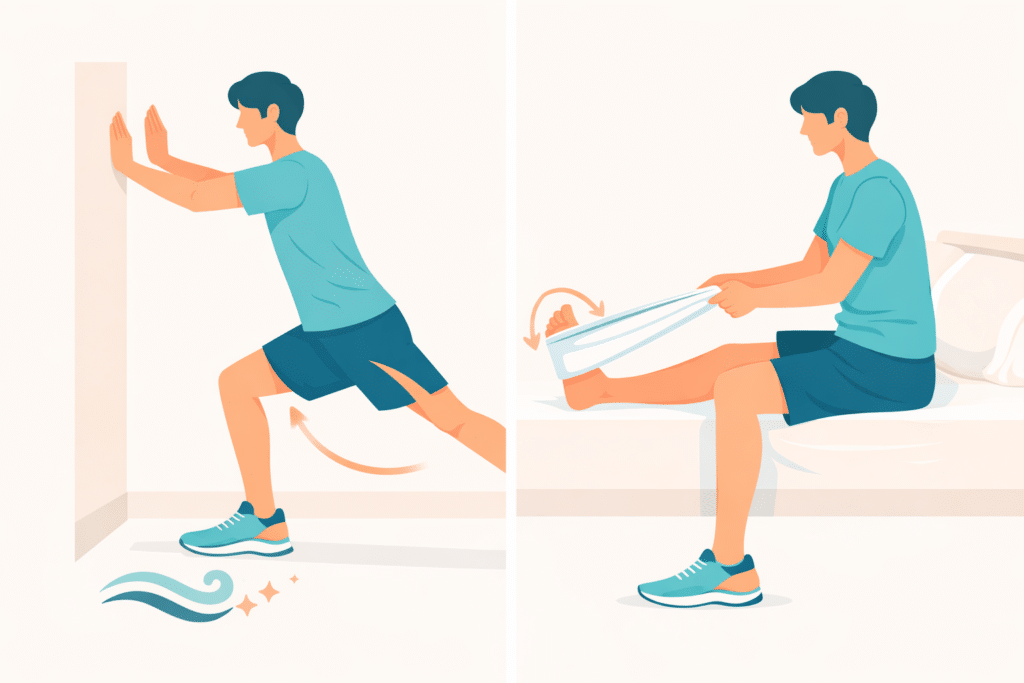
Standing wall calf stretch + seated towel stretch
Reference:
Harvard Health: Stretching to help plantar fasciitis
6) When Slippers Aren’t Enough
If your heel pain is flaring hard, slippers might not be structured enough — even supportive ones.
And if your footwear is old and flattened out, that may be part of the problem. See our 2026 Guide: When to Replace Your Plantar Fasciitis Shoes.
That’s when many people do better wearing a more supportive shoe indoors (like a stable sneaker with inserts) until things calm down.
- Severe morning pain: consider discussing options like night splints with a professional.
- Constant flare-ups: indoor support + stretching + better outdoor footwear usually need to work together.
FAQ: Slippers & House Shoes for Plantar Fasciitis
Q: Are slippers actually helpful for plantar fasciitis?
A: Yes — if they provide real arch support and heel stability. Supportive slippers reduce repeated strain from barefoot walking on hard floors.
Q: Are backless slippers (mules) a bad idea?
A: Often, yes. Many people “toe-grip” to keep them on, which can irritate the foot. A secure upper or strap is usually better.
Q: Should I wear supportive slippers all day at home?
A: If your floors are hard and you’re on your feet often, wearing supportive indoor footwear is usually a smart move — especially during flare-ups.
Q: When should I replace my slippers?
A: When the footbed flattens, the heel feels less stable, or your pain creeps back. If the support collapses, your heel notices.
Q: When should I see a healthcare professional?
A: If pain is severe, persistent, or not improving with supportive changes and basic home care, it’s time to get evaluated.
Wrap-Up: Make Home the Place Your Heels Recover
If plantar fasciitis is flaring, barefoot-at-home is usually gasoline on the fire.
Supportive slippers and house shoes give your foot consistent arch support and heel stability — and consistency is what helps your heel settle down.
Next steps:
Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
and, if you want the broader relief plan,
Healing Plantar Fasciitis Naturally: 5 Proven Home Remedies for Fast Relief.
Medical Disclaimer: Bob and Lisa are not doctors. We’re sharing personal experience and practical, empathy-first guidance.
For medical advice, diagnosis, or treatment plans, please consult a qualified healthcare professional.
We reference reputable sources (like Mayo Clinic, Cleveland Clinic, and Harvard Health) for general education.

