The Bottom Line: Insoles Basics for Relieving Plantar Fasciitis Pain
Insoles relieve pain because they reduce strain on the plantar fascia by supporting your arch, stabilizing your foot, and cushioning your heel.
For many people, the right insoles make walking more tolerable quickly—especially when combined with supportive shoes and a simple stretching routine.
The key is choosing an insole with real arch support and a deep, stable heel cup (not just a squishy pad).
Disclosure: This post may contain affiliate links. If you buy through them, we may earn a small commission at no extra cost to you.
“We understand your pain” is not hyperbole…
If you’ve ever had plantar fasciitis, you know the special kind of rage it can trigger. You’re not “being dramatic.”
It genuinely feels like someone drove a thumbtack into your heel and then dared you to go live a normal life.
Here’s the good news: insoles are one of the fastest “first upgrades” you can make—because they change what your foot is doing
every single time you take a step. And steps add up fast.
Want the bigger picture? See our full footwear guide here:
Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
1) What an Insole Actually Does
Plantar fasciitis is often aggravated by repeated stress on the plantar fascia (that thick band of tissue under your foot).
Insoles can help by changing how force moves through your foot and heel when you stand and walk.
Credible medical overviews explain that supportive measures (including orthotics/insoles) are commonly used as part of treatment.
Think of a good insole as doing three jobs:
- Arch support: helps reduce “overstretching” and strain through the midfoot.
- Heel stabilization: a deep heel cup can reduce wobble and keep the foot more aligned.
- Cushioning: softens impact under the heel (especially helpful on hard floors).
Reference: Cleveland Clinic: Plantar Fasciitis
2) The #1 Mistake: Buying “Soft” Instead of Buying “Support”
Most people start by grabbing the softest, squishiest insert they can find. Totally understandable.
The problem is: squish alone doesn’t guide your foot.
You want a blend of cushioning and structure—especially a stable heel cup and real arch shape.
The American Orthopaedic Foot & Ankle Society (FootCareMD) highlights supportive footwear and common conservative measures used to relieve plantar fasciitis symptoms.
3) Over-the-Counter vs Custom Orthotics
Here’s our take, based on what tends to work for real people spending real money:
- Over-the-counter (OTC) insoles are often a great first step—especially if you choose a structured, reputable option.
Many folks get meaningful relief without going custom. - Custom orthotics can help in specific cases (foot structure issues, persistent pain, unusual gait mechanics),
but they’re usually not the first thing you need to try.
If pain is severe, persistent, or keeps coming back despite good shoes + good insoles, it’s worth getting evaluated by a professional.
Reference: Cleveland Clinic: Plantar Fasciitis
4) What to Look For in Plantar Fasciitis Insoles
Use this like a “don’t get ripped off” checklist:
- Deep heel cup: helps stabilize the heel and reduce sloppy motion.
- Firm-to-medium arch support: should feel supportive, not like a flat sponge.
- Correct length: full-length for athletic shoes, 3/4 length for tighter dress shoes (sometimes).
- Material that matches your needs: more cushion if impact hurts; more structure if stability is the issue.
Action Box: The 60-Second Insole Reality Check
- [ ] Does the insole have a deep heel cup (not just padding)?
- [ ] Can you feel a real arch shape that matches your foot?
- [ ] Does it feel stable when you stand—like your heel isn’t wobbling?
- [ ] Will it actually fit your shoe without cramming your toes?
- [ ] Are you willing to “break it in” for a few days instead of rage-quitting on Day 1?
5) How to Fit and Break In Insoles (So You Don’t Hate Them)
Insoles aren’t always “love at first step.” A little break-in is normal—especially if you’ve been walking unsupported for a while.
- Day 1–2: wear them 1–2 hours, then rest.
- Day 3–4: increase to half a day if they feel okay.
- After that: build toward full-day wear.
If insoles cause sharp new pain, numbness, or make you limp more, stop and reassess fit/support level.
(This is also where a medical professional can help.)
6) Our Go-To Insole Options
These are commonly used brands/options people turn to for plantar fasciitis support.
- Premium support (structured): Superfeet
- Balanced support + cushioning: PowerStep
- Budget-friendly starter option: Dr. Scholl’s Dr. Scholl’s sells a lot of products that are strictly comfort. Make certain they are orthotics, for plantar fasciitis, and look at weight rating.
- Adjustable-style insert: WalkFit
Important: even the best insoles struggle if your shoes are worn out or too flimsy. Pair insoles with supportive footwear.
7) Helpful “Extras” (Optional, Don’t Overdo It)
If your pain is intense, it’s normal to want more than one tool in the toolbox. Here are a few that many people find helpful:
- Night splint: keeps the foot gently flexed so the first step in the morning is less brutal.
- Foot massage roller: easy, cheap, and good for daily relief.
- Orthotic slippers for indoors: because barefoot-on-hard-floor is basically plantar fasciitis’s favorite hobby.
If hard floors are part of your problem, see our Slippers for Plantar Fasciitis 2026: Cozy Support That Saves Your Heels at Home.
8) Yes, Stretching Still Matters (Quick + Simple)
Insoles help during activity. Stretching helps reduce the “pull” that keeps aggravating the fascia.
Harvard Health has a simple overview of plantar fasciitis stretching approaches here:
Reference: Harvard Health
If you want more step-by-step stretching help, see our Effective Stretches for Heel Pain Relief: Step-by-Step.
- Standing wall calf stretch: 15–30 seconds per side, 2–3 rounds.
- Seated towel stretch: gentle pull, 15–30 seconds per side.
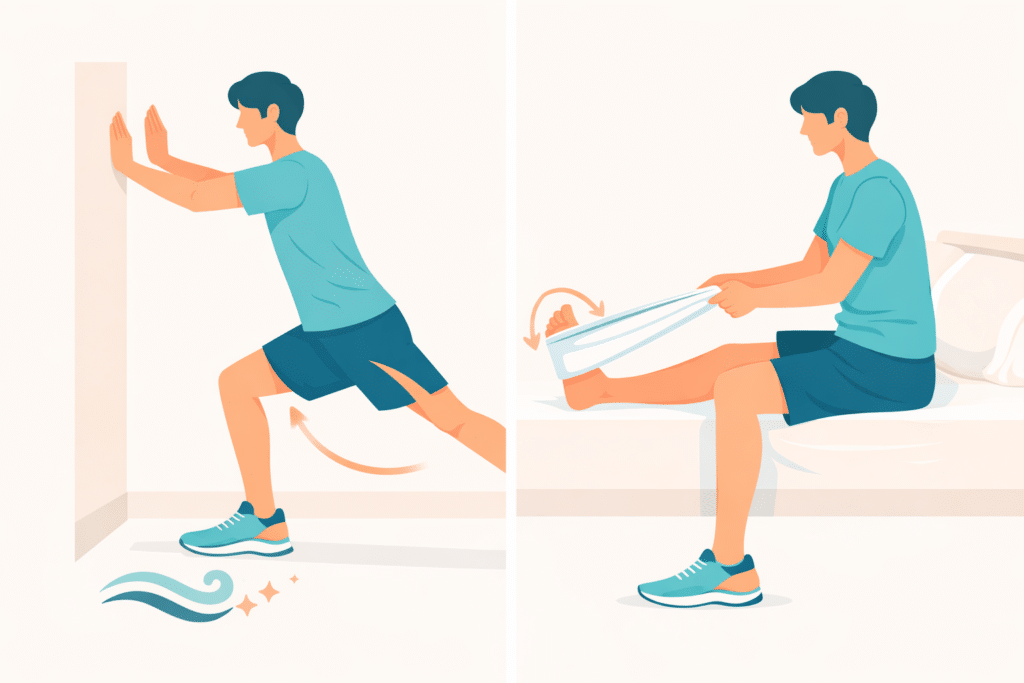
Standing wall calf stretch + seated towel stretch
FAQ: Insoles and Plantar Fasciitis
Q: Do insoles cure plantar fasciitis?
A: They can reduce strain and pain for many people, but they’re usually one part of a bigger plan (support + stretching + smart activity). If symptoms persist, get evaluated.
Q: How long does it take to feel relief?
A: Some people feel improvement quickly, others need a couple of weeks—especially if they’re also fixing footwear and doing basic stretches.
Q: Should I wear insoles in every shoe?
A: Ideally, yes—because inconsistent support can keep re-irritating the fascia. At minimum, wear them in the shoes you use most.
Q: Can I use insoles if I stand all day?
A: Yes—just be extra picky about stability and heel support, and replace insoles when they compress and flatten out.
Q: When should I replace insoles?
A: If arch support collapses, heel cup feels mushy, or pain creeps back, it’s probably time. Heavy use often means replacing sooner.
Q: When is it time to see a doctor?
A: If pain is severe, lasts more than a few weeks despite supportive changes, or you have numbness/tingling, diabetes, or significant swelling—get medical guidance.
Wrap-Up
If plantar fasciitis is ruining your days, insoles can be one of the fastest ways to make walking less miserable—because they support your foot with every step.
Start with structure (arch + heel cup), fit them properly, break them in, and pair them with supportive footwear.
Next steps:
Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
and (if you want a broader healing plan)
Healing Plantar Fasciitis Naturally: 5 Proven Home Remedies for Fast Relief
Medical Disclaimer: Bob and Lisa are not doctors. We’re sharing personal experience and practical, empathy-first guidance.
For medical advice, diagnosis, or treatment plans, please consult a qualified healthcare professional.
We reference reputable sources like Mayo Clinic, Cleveland Clinic, Harvard Health, and FootCareMD for general education.

