Quick Answer: Insoles Can Help Plantar Fasciitis — If They Support, Not Just Cushion
Plantar fasciitis orthotic insoles can help reduce heel pain by supporting your arch, stabilizing your heel, and softening impact when you stand or walk. The best first upgrade is usually a structured insole with a real arch shape and a deep heel cup — not a flat, squishy pad that feels nice for five minutes and then gives up like a lawn chair in a thunderstorm.
Disclosure: This post may contain affiliate links. If you buy through them, we may earn a small commission at no extra cost to you.
Medical note: This guide is educational and based on personal experience plus reputable medical sources. It is not medical advice. If your heel pain is severe, worsening, or not improving, please check with a qualified healthcare professional.
Insoles Basics for Plantar Fasciitis: Start Here Before You Spend Big
If you’ve ever had plantar fasciitis, you know the special kind of fury it can inspire. You are not “being dramatic.” When every step feels like your heel is negotiating with a thumbtack, normal life gets annoying fast.
The good news: insoles are one of the fastest first upgrades many people can try because they change what your foot is doing every time you stand, walk, climb stairs, run errands, or wander into the kitchen looking for snacks like a wounded raccoon.
The trick is knowing what you’re buying. A good insole supports your foot. A bad one is just a soft rectangle with marketing copy.
Want the full footwear plan? Start with our hub guide: Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide.
This Guide Is for You If…
- You have heel pain and suspect your shoes are not giving enough support.
- You’re overwhelmed by the difference between insoles, inserts, and orthotics.
- You want to try over-the-counter support before paying for custom orthotics.
- You stand, walk, or work on hard floors and your heels are filing complaints.
- You need a simple checklist for choosing plantar fasciitis insoles without getting lost in product hype.
1) What an Insole Actually Does
The plantar fascia is the thick band of tissue running along the bottom of your foot. When it gets irritated, every step can tug on an already angry structure. Supportive insoles can help by changing how force moves through your foot and heel.
Think of a good plantar fasciitis insole as doing three jobs:
- Arch support: helps reduce excessive strain through the midfoot.
- Heel stabilization: a deep heel cup helps keep your heel from wobbling around like it has its own agenda.
- Cushioning: helps soften impact under the heel, especially on hard floors or during long walking days.
Medical sources commonly include orthotics, arch supports, supportive shoes, stretching, icing, and other conservative measures in plantar fasciitis care. Cleveland Clinic specifically recommends sturdy, well-cushioned shoes and avoiding bare feet, while Mayo Clinic notes that arch supports or orthotics can help distribute pressure more evenly across the feet.
References: Cleveland Clinic: Plantar Fasciitis | Mayo Clinic: Plantar Fasciitis Diagnosis & Treatment
2) The #1 Mistake: Buying Soft Instead of Buying Support
Most people start by grabbing the softest insert they can find. Understandable. When your heel hurts, soft feels like the obvious hero.
But for plantar fasciitis, soft alone is usually not enough. A squishy insert may cushion impact, but if it does not support your arch or stabilize your heel, your plantar fascia may still get yanked around all day.
Bob/Lisa translation: comfort is nice. Structure is what keeps your foot from staging a rebellion.
PF-Friendly Insole Formula
Support first. Cushion second. Fit always. If an insole has no arch shape, no heel cup, and makes your shoe too tight, it is probably not your foot’s new best friend.
3) Insoles, Inserts, and Orthotics: What’s the Difference?
People use these words interchangeably, which is why shopping for foot support can feel like decoding a goblin treaty. Here’s the simple version:
- Inserts: a broad term for anything you add inside a shoe.
- Insoles: removable footbeds or support layers that improve cushioning, fit, or structure.
- Orthotics: support devices designed to correct or improve foot mechanics. These can be over-the-counter or custom-made.
For this article, we’re mostly talking about over-the-counter plantar fasciitis orthotic insoles — the structured inserts you can buy without a prescription.
4) Over-the-Counter vs. Custom Orthotics
Here’s our practical take:
- Over-the-counter insoles are often a sensible first step if you choose a reputable, structured option with arch support and a heel cup.
- Custom orthotics may help when pain is persistent, your foot structure is unusual, you have gait issues, or a clinician recommends them.
In other words, don’t assume “custom” is automatically your first move. But don’t ignore professional help if the cheap-and-simple fixes are not working.
If pain is severe, keeps returning, changes your gait, or comes with numbness, tingling, swelling, or other unusual symptoms, get evaluated. Your foot is not a mystery novel. You do not get bonus points for refusing clues.
5) What to Look For in Plantar Fasciitis Insoles
Use this like a “don’t get fooled by squishy packaging” checklist:
- Deep heel cup: helps stabilize the heel and reduce sloppy motion.
- Firm-to-medium arch support: should feel supportive, not like a flat sponge.
- Heel cushioning: helpful for impact, especially if hard floors or long walks trigger pain.
- Correct length: full-length for many athletic and walking shoes; 3/4 length may work better in tighter dress shoes.
- Good shoe fit: the insole should not cram your toes, lift your heel out of the shoe, or make you walk strangely.
- Replaceable design: if the support flattens, the insole has done its tour of duty and should retire with honors.
Action Box: The 60-Second Insole Reality Check
- [ ] Does the insole have a deep heel cup, not just padding?
- [ ] Can you feel a real arch shape that matches your foot?
- [ ] Does your heel feel stable when you stand?
- [ ] Does it fit your shoe without cramping your toes?
- [ ] Does it support your foot without creating sharp new pain?
- [ ] Are you willing to break it in gradually instead of rage-quitting on Day 1?
6) How to Fit and Break In Insoles
Insoles aren’t always love at first step. A short break-in period is normal, especially if you’ve been walking around with minimal support for a long time.
- Day 1–2: wear them for 1–2 hours, then switch back if your feet feel tired.
- Day 3–4: increase to half a day if they feel okay.
- After that: build toward full-day wear.
Stop and reassess if the insole causes sharp pain, numbness, tingling, new knee/hip pain, or makes you limp more. That may mean the arch is wrong for you, the insole is too aggressive, or your shoe fit is off.
Bob/Lisa rule: support should feel firm and useful — not like your shoe hired a tiny dictator to bully your arch.
7) Our Go-To Insole Starting Points
These are common over-the-counter insole brands people look at when they want more structure for plantar fasciitis. We are not saying one brand is perfect for every foot. Feet are weird little kingdoms. The right option is the one that fits your arch, shoe, activity level, and comfort tolerance.
As an Amazon Associate, we earn from qualifying purchases.
- Premium support / structured feel: Superfeet
- Balanced support + cushioning: PowerStep
- Budget-friendly starter option: Dr. Scholl’s plantar fasciitis orthotics
- Adjustable-style insert: WalkFit
Shopping note: Dr. Scholl’s sells many comfort products, not all of which are true plantar fasciitis orthotics. Make sure the product is meant for plantar fasciitis support, check sizing/weight guidance, and avoid anything that is just soft foam with no structure.
Important: even the best insoles struggle if your shoes are worn out, flimsy, or too tight. Pair insoles with supportive footwear, not ancient sneakers that belong in a footwear museum.
8) Helpful Extras: Don’t Turn Your Living Room Into a Foot Clinic
If your pain is intense, it’s normal to want more than one tool in the toolbox. Just don’t try five new things on the same day, or you won’t know what helped and what made your foot file a formal complaint.
- Night splint: may help with first-step morning pain by keeping the foot gently positioned overnight.
- Foot massage roller: useful for gentle daily rolling if that gives you relief.
- Orthotic slippers for indoors: helpful if hard floors are part of your problem.
If hard floors are aggravating your heel, see our indoor footwear guide: Slippers for Plantar Fasciitis 2026: Cozy Support That Saves Your Heels at Home.
9) Yes, Stretching Still Matters
Insoles help while you are standing and moving. Stretching helps reduce the tug-of-war on the plantar fascia and calf chain. Medical sources commonly include stretching as part of conservative plantar fasciitis care.
Reference: Harvard Health: Stretching to help plantar fasciitis
Simple starting points:
- Standing wall calf stretch: 15–30 seconds per side, 2–3 rounds.
- Seated towel stretch: gentle pull, 15–30 seconds per side.
- Frozen bottle roll: gentle rolling for short sessions if it feels good.
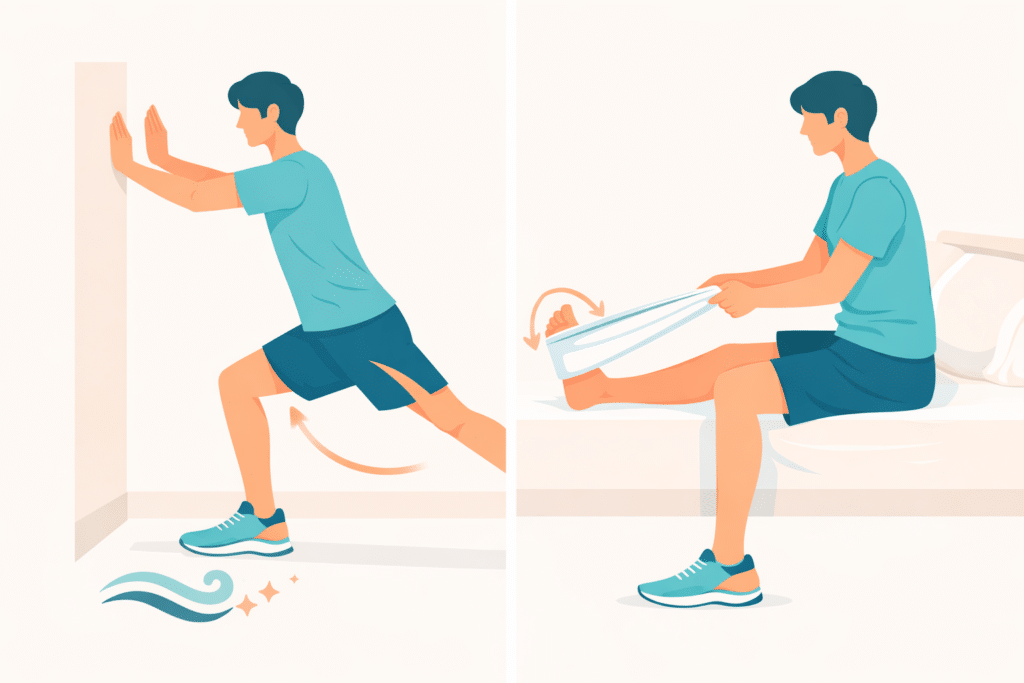
Standing wall calf stretch + seated towel stretch
If you want more step-by-step stretching help, see our guide: Effective Stretches for Heel Pain Relief: Step-by-Step.
10) When Insoles Are Not Enough
Insoles are useful, but they are not magic. They work best as part of a simple system:
- Supportive shoes outside the house.
- Supportive slippers or house shoes inside the house.
- Structured insoles when your shoes need more arch or heel support.
- Stretching and gentle recovery habits.
- Professional evaluation when pain is persistent, severe, or unusual.
If your shoes are old, the insole may not save them. See: 2026 Guide: When to Replace Your Plantar Fasciitis Shoes.
Recommended Next Reads
- Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
- Athletic Shoes for Plantar Fasciitis
- Slippers for Plantar Fasciitis 2026
- When to Replace Your Plantar Fasciitis Shoes
- Healing Plantar Fasciitis Naturally: 5 Proven Home Remedies for Fast Relief
FAQ: Insoles and Plantar Fasciitis
Q: Do insoles cure plantar fasciitis?
A: No insole can honestly promise a cure. But structured insoles can reduce strain and pain for many people when used with supportive shoes, stretching, and smart activity habits.
Q: What are the best insoles for plantar fasciitis?
A: Look for insoles with real arch support, a deep heel cup, firm-to-medium structure, and enough heel cushioning for your activity level. The best insole is the one that fits your foot and shoe without creating new pain.
Q: Are soft gel inserts good for plantar fasciitis?
A: They may feel comfortable, but soft gel alone usually does not provide enough structure. For plantar fasciitis, support plus cushioning usually beats cushioning alone.
Q: Should I wear insoles in every shoe?
A: Ideally, use consistent support in the shoes you wear most. Switching between supported shoes and flat, unsupportive shoes can keep re-irritating the plantar fascia.
Q: How long does it take to feel relief from insoles?
A: Some people feel improvement quickly. Others need a couple of weeks, especially while breaking in the insole and fixing footwear habits. If pain worsens, stop and reassess.
Q: Can insoles help if I stand all day?
A: Yes, they can help, but shoe quality matters too. If you stand on concrete or hard floors, look for supportive shoes plus structured insoles and replace both when support collapses.
Q: When should I replace my insoles?
A: Replace them when the arch support flattens, the heel cup feels mushy, the top cover wears out, or your heel pain starts creeping back despite no other obvious change.
Q: When should I see a doctor or podiatrist?
A: Get medical guidance if pain is severe, lasts more than a few weeks despite supportive changes, affects your walking, or comes with numbness, tingling, swelling, diabetes, or a new injury.
Wrap-Up: Start With Structure
If plantar fasciitis is making every step miserable, insoles can be one of the simplest ways to give your foot more support. Start with the basics: arch support, deep heel cup, stable fit, and shoes that are worth supporting in the first place.
Then build the rest of the system: supportive footwear, indoor slippers, simple stretches, and smarter replacement habits. That’s not glamorous. But neither is limping to the coffee pot like you lost a duel with the kitchen floor.
Next step: Return to the main footwear guide here: Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide.
Medical Disclaimer: Bob and Lisa are not doctors. We’re sharing personal experience and practical, empathy-first guidance. For medical advice, diagnosis, or treatment plans, please consult a qualified healthcare professional. We reference reputable sources such as Mayo Clinic, Cleveland Clinic, Harvard Health, and other medical education resources for general education.

