Disclosure: This post may contain affiliate links. If you buy through them, we may earn a small commission at no extra cost to you.
The Bottom Line: Boots Don’t Have to Equal Heel Torture
If you have plantar fasciitis, the right boots protect your heel by supporting your arch, stabilizing your foot, and cushioning impact—while keeping you warm and upright.
The key is choosing boots with real structure (not just “soft”), room for supportive insoles, and traction you can trust.
When sneaker weather disappears, a lot of people with plantar fasciitis do the same sad math:
Cold + boots = stiff, flat, angry feet.
And yeah… some boots are basically foot armor with the arch support of a pancake.
But here’s the good news: there are winter boots and hiking boots that can handle cold, traction, and trails without turning your plantar fascia into a screaming rubber band.
You just need to know what matters (and what’s a marketing mirage).
Want the bigger picture? See our main footwear guide here:
Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
1) What Your Plantar Fascia Needs From a Boot
Plantar fasciitis is often aggravated by repeated strain and impact—especially on hard surfaces, uneven ground, and long days on your feet.
Major medical sources consistently point to supportive footwear, stretching, and (when appropriate) inserts/orthotics as common parts of conservative treatment.
For boots, that translates into four non-negotiables:
- Arch support (or removable insoles): You want a boot that supports the midfoot—or at least lets you insert a supportive insole/orthotic.
- Heel stability: A stable heel cup + firm rear structure helps reduce sloppy motion that can irritate the fascia.
- Cushioning (but not “mushy”): Enough shock absorption to reduce heel strike pain—without turning your boot into a wobble-factory.
- Traction: Slipping on ice or sliding on loose gravel makes your foot tense and land weird. That’s not a fun hobby for plantar fasciitis.
References:
Mayo Clinic: Plantar fasciitis diagnosis & treatment,
Cleveland Clinic: Plantar fasciitis
2) The Classic Boot Mistakes That Trigger Flare-Ups
Most plantar fasciitis boot regret comes from one of these:
- Too flat: Completely flat boots can increase the tug on your plantar fascia—especially if your calves/Achilles are tight.
- Too stiff in the wrong place: A boot that won’t bend at the forefoot forces your foot to work harder with every step.
- No room for support: If you can’t fit a supportive insert, your boot is basically “winter pain storage.”
- Worn-out insoles: Even decent boots can become PF-hostile once the footbed collapses.
Action Box: The 60-Second Boot Reality Check
- [ ] Does the boot have real arch shape or allow a supportive insole?
- [ ] Does the heel feel stable (not wobbly or sloppy)?
- [ ] Is there cushioning under the heel without feeling like a marshmallow?
- [ ] Can you wiggle your toes, especially going downhill?
- [ ] Does the outsole have traction you’d trust on wet/icy surfaces?
3) Winter Boots vs Hiking Boots: What to Prioritize
Winter boots should keep you warm and upright. That means insulation + traction + a supportive platform.
Hiking boots should keep you stable on uneven terrain. That means a stable midsole + secure fit + room for support.
A) Winter boots (snow, ice, sidewalks)
- Look for: traction-first outsole, stable heel, removable footbed if possible, enough volume for an insole.
- Avoid: flat “fashion boots” with thin soles and no structure.
Popular winter boot options people often consider:
- Orthotic-friendly winter boot: OrthoFeet winter boots
- Insulated trail-style winter boot: Merrell Thermo series
- Wide-foot friendly winter option: winter boots available in wide sizes
B) Hiking boots (trails, rocks, uneven terrain)
- Look for: stable midsole, heel lockdown, enough toe room for descents, and a removable insole (so you can upgrade support).
- Avoid: boots that feel “twisty” underfoot or collapse inward when you stand.
Popular hiking boot options people often consider:
- Stability-forward hiking boot: Salomon X Ultra series
- Budget-friendly day-hike boot: Columbia Newton Ridge
- Roomy toe box hikers: KEEN hiking boots and other wide-toe options
4) Fitting Boots for Heel & Arch Relief (This Matters More Than Brands)
The fit is where plantar fasciitis success or failure happens—especially with hiking boots.
You want a secure heel (less slipping), enough forefoot room (especially downhill), and enough volume for support.
- Try boots on later in the day: feet swell a bit; if they fit then, you’re safer.
- Bring your inserts/orthotics: boots and inserts are a “unit,” and inserts take up space.
- Heel lift can help some people: a small heel-to-toe drop may reduce strain if your calves are tight (totally individual).
It’s also normal to need an adjustment period when introducing new inserts/support.
If you need help choosing inserts, see our Insoles Basics for Plantar Fasciitis guide.
Reference:
FootCareMD: Orthotics (break-in and fitting considerations)
5) Break In Rules (So You Don’t Rage-Quit on Day 1)
Boots and supportive inserts can feel “different” at first—especially if your feet have been living unsupported for a while.
A gradual break-in often works better than jumping into a long walk or hike immediately.
- Day 1–2: 30–90 minutes indoors or short errands.
- Day 3–4: half-day wear if it feels okay.
- After that: build toward longer walks/hikes.
Stop and reassess if you get sharp new pain, numbness/tingling, or you start limping more.
That’s your body saying “nope”—and it’s worth adjusting fit/support or getting professional guidance.
6) Helpful “Extras” for Cold + Trails (Optional, Don’t Overdo It)
If your plantar fasciitis flares easily, it’s normal to want a bigger toolbox.
Common conservative treatment guidance includes things like stretching, night splints, and inserts/orthotics.
- Supportive insoles: a structured insert can upgrade a boot fast.
- Night splint: can reduce morning pain for some people.
- Foot roller / massage ball: easy daily relief tool.
- Supportive indoor slippers: because barefoot on hard floors is plantar fasciitis’s favorite hobby.
Bob note: I know night splints look scary, but they’re relatively cheap and they worked miracles for me. Lisa couldn’t get used to sleeping with them on. Lisa still keeps a foot roller under her desk just “because.” And my “barefoot beach bunny” never got over plantar fasciitis until she finally started wearing orthotic slippers around the house.
And if hard floors are part of your problem after you get home (like they were for Lisa), see our Slippers for Plantar Fasciitis 2026: Cozy Support That Saves Your Heels at Home.
References:
Mayo Clinic,
Cleveland Clinic
7) Yes, Stretching Still Matters (Especially If You Hike)
Boot support helps during activity. Stretching helps reduce the “pull” that keeps aggravating the fascia—especially if your calves and Achilles are tight.
Harvard Health notes stretching as part of common conservative management, including calf stretches and plantar fascia-specific stretches.
Reference:
Harvard Health: Plantar fasciitis symptoms, causes, and treatments
- Standing wall calf stretch: 15–30 seconds per side, 2–3 rounds.
- Seated towel stretch: gentle pull, 15–30 seconds per side.
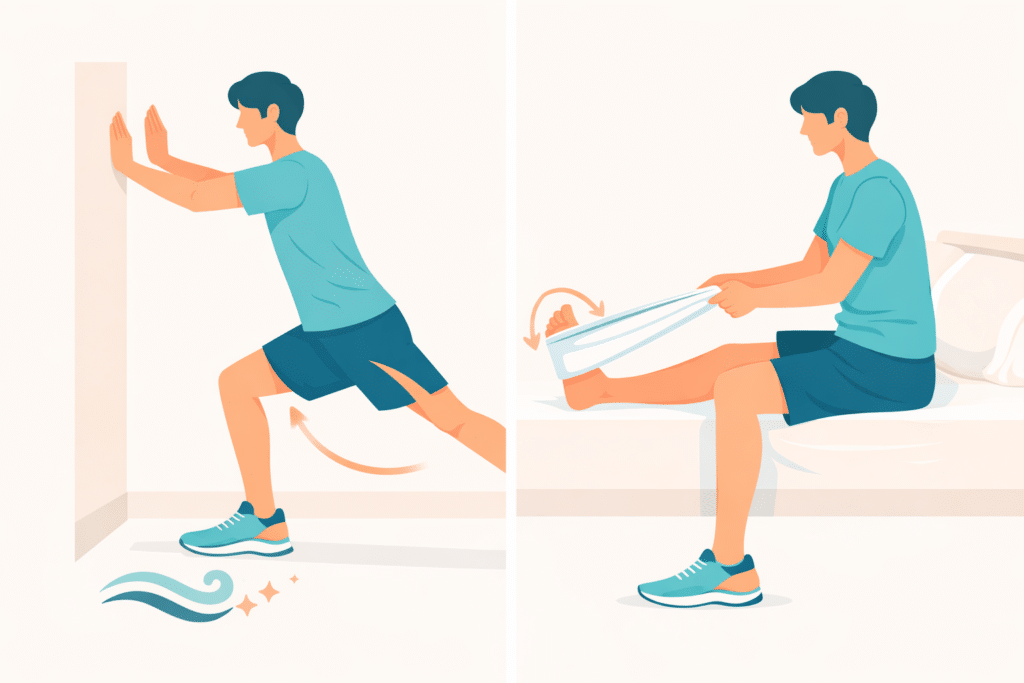
Standing wall calf stretch + seated towel stretch
If you want a more detailed stretching routine, see our Effective Stretches for Heel Pain Relief: Step-by-Step.
FAQ: Hiking Boots & Plantar Fasciitis
Q: Do hiking boots help plantar fasciitis?
A: They can—if they’re supportive and stable. A boot that supports the arch (or accepts a supportive insert) and keeps the heel steady is often better than a flat, flimsy option.
Q: Are “soft” boots better for heel pain?
A: Not always. Cushioning helps, but you usually need structure too. Too-mushy boots can increase wobble and irritation.
Q: What if I need boots for icy sidewalks?
A: Traction matters. Slipping changes how you land and can trigger flare-ups. Prioritize a grippy outsole and a stable heel platform.
Q: Should I put orthotics in hiking boots?
A: Many people do. Just make sure the boot has enough volume and your heel stays locked in. Plan for a break-in period.
Q: When should I see a doctor?
A: If pain is severe, lasts more than a few weeks despite supportive changes, or you have numbness/tingling, diabetes, or significant swelling—get medical guidance.
Wrap-Up: Conquer the Cold & Trail, Sans Heel Scream
You don’t have to let plantar fasciitis cancel winter or the outdoors.
Get boots that prioritize support + stability + traction, make room for a supportive insole if needed, and break them in like a civilized human (not like you’re storming a mountain on Day 1).
Next steps:
Best Footwear for Plantar Fasciitis 2026: The Ultimate Guide
and (for a broader plan)
Healing Plantar Fasciitis Naturally: 5 Proven Home Remedies for Fast Relief
Medical Disclaimer: Bob and Lisa are not doctors. We’re sharing personal experience and practical, empathy-first guidance.
For medical advice, diagnosis, or treatment plans, please consult a qualified healthcare professional.
We reference reputable sources (like Mayo Clinic, Cleveland Clinic, Harvard Health, and FootCareMD) for general education.

